Suboxone (buprenorphine) creates a physical dependence in the brain. Stopping cold turkey usually leads to withdrawal symptoms. By slowly taking less and less of the medication, patients can come off Suboxone (or Subutex) within weeks or months without unpleasant symptoms.
Skip To
Suboxone Withdrawals | Taper Guide | Patient Advice | Medications | Ask a Question
Suboxone Withdrawal Symptoms
Suboxone and Subutex are partial opioids, so withdrawal symptoms are similar but milder than withdrawal from opioids like prescription pain medications or heroin.
- Low energy
- Loss of appetite
- Irritability
- Muscle weakness
- Withdrawal insomnia / Restlessness
Physical Symptoms of Suboxone Withdrawal
A tapering schedule reduces or eliminates these symptoms. No reduction in medication should be attempted until all physical withdrawal has subsided from the last dosage reduction.
Mental Symptoms of Suboxone Withdrawal
The most common mental symptoms of withdrawal are anxiety and depression.
That is why it's so important to keep up with MAT individual and group therapy sessions. Treating all the behaviors and emotions that are unique to you will make a lasting and successful recovery possible. It is also helpful to maintain a healthy diet and a good daily routine or work schedule; exercise can be very beneficial as well.
Suboxone Taper & Relapse
Another side effect of a Suboxone taper is relapse. If cravings become intense after tapering, Vivitrol may offer a safety net.
While you may want to move off Suboxone quickly, being so uncomfortable in a taper that relapse occurs is the opposite of the goal.
How Long Does Suboxone Withdrawal Last?
Symptoms can last from a few days to several weeks. Generally, symptoms start within 48 hours after the last dose and peak around day three.
Some patients experience mental health symptoms for weeks or months after opioid/Suboxone use, which is known as Post-Acute Withdrawal Syndrome (PAWS).
A slow taper off of Suboxone helps prevent PAWS and minimizes the severity of all withdrawal symptoms.
The Standard Suboxone Taper Schedule
It is best to work with your doctor to create a tapering schedule that is most effective for your total recovery and based on clinic requirements.
A general guideline: reduce daily dose by 10% to 20% every one to two weeks.
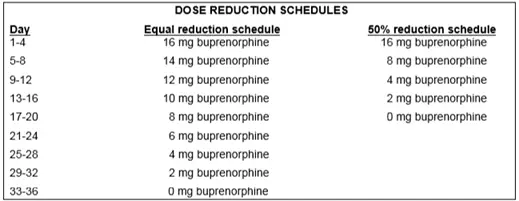
- NOTE: These guidelines are more aggressive than what is ideal for most people.
How to Taper Off Suboxone: According to Patients
"The best advice I can give is to start with a plan, listen to your body and take your time. It gets harder at lower doses, but you’ll get there."
"I was on 8mg of Suboxone for 5 years. I tapered very slowly. Exercise and lots of water help."
"I recommend tapering down very slowly. You will eventually get off and avoid feeling sick."
Medications to Get Off Suboxone
Suboxone to Sublocade
Sublocade is a long-acting injection of buprenorphine given monthly. It may reduce withdrawal symptoms and daily cycle frustrations.
"I switched to Sublocade. It’s been 12 weeks since my last shot, no withdrawals yet."
Suboxone to Kratom (Don't Do It)
Kratom is marketed as natural but acts on opioid receptors and causes similar withdrawal symptoms.
Research shows:
"I got addicted to Kratom after being clean off heroin. Then I relapsed."
Suboxone to Vivitrol
Vivitrol is a monthly naltrexone shot, used only after fully tapering off Suboxone. It is non-addictive and doesn’t cause withdrawal when stopped. More info here.
Suboxone to Methadone
Methadone is habit-forming, requires more in-person visits, and may not support the goal of reducing medications. However, the switch is straightforward. See details.
Need Help With Your Suboxone Detox?
Our Medication-Assisted Treatment (MAT) doctors can help you taper off Suboxone quickly and comfortably.

