Suboxone: What Is Suboxone? How Does It Work?
Suboxone was developed as an alternative to methadone to ease the severe symptoms of opioid withdrawal and help with ongoing cravings. If an individual has a strong desire to stop taking opioids but has intense cravings, they are likely a candidate for a Suboxone program.
Skip To
What Is Suboxone | How It Works | How to Take It | Is It Right For Me? | Ask A Question
What Is Suboxone?
Suboxone has been FDA-approved to treat opioid use disorder since 2002. It is a sublingual film that dissolves under the tongue with a combination of two medications – buprenorphine and naloxone. Suboxone diminishes withdrawal symptoms and cravings for opioids.
Suboxone Is A Partial Opioid
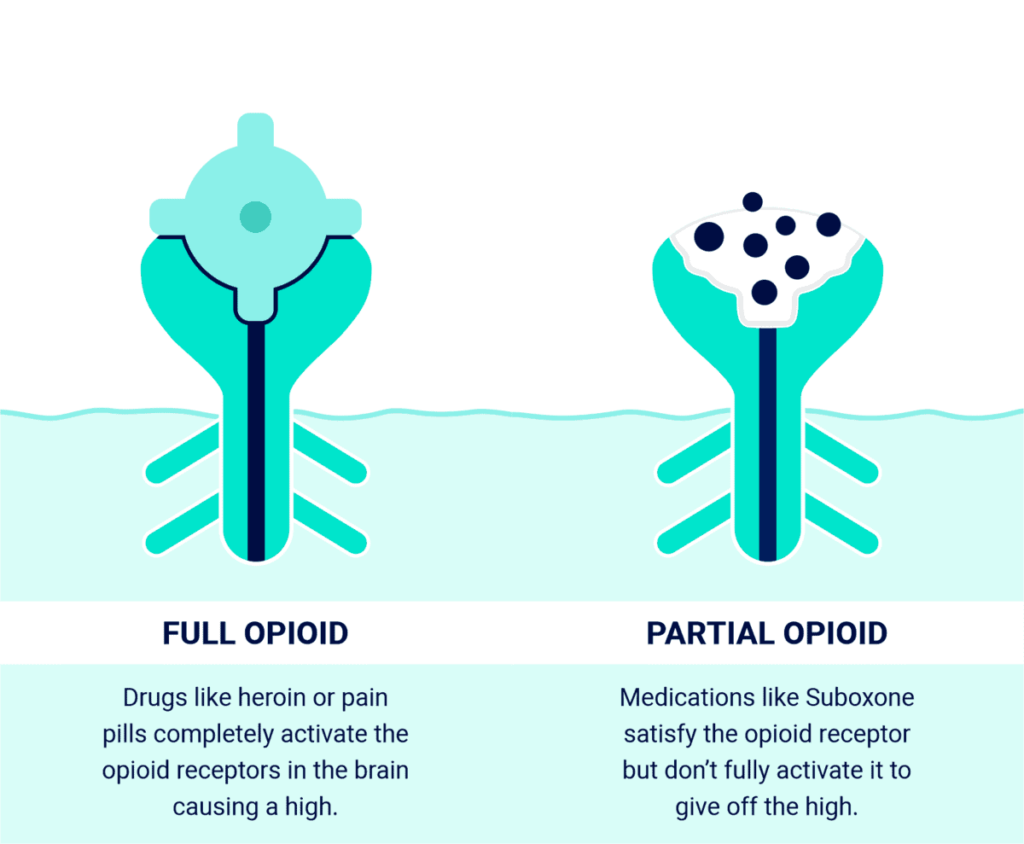
- NOTE: Suboxone is not the same medication as methadone or Vivitrol (Naltrexone). See Suboxone vs. Methadone or Vivitrol vs. Suboxone.
FAQs: What is Suboxone?
Is Suboxone An Opioid?
Yes, Suboxone is an opioid because it attaches to opioid receptors in the brain, but it does not fully activate them. Suboxone is safer than other opioids like oxycodone or heroin since it is only a partial opioid agonist.
Is Suboxone a Controlled Substance?
Yes, Suboxone is a Schedule III controlled substance because it has a “moderate to low” potential for abuse and addiction. Suboxone doctors must have a specific license and are monitored by the D.E.A.
How Does Suboxone Work?
Suboxone works by blocking the receptors in the brain that crave opioids, without activating these receptors to create a “high.” Blocking opioid receptors stops the brain from sending signals that cause withdrawal symptoms and cravings for opioids. If drugs like heroin or prescription pain pills are used, the opioid receptors are blocked, so these drugs will not give off the “high” either.
Suboxone Ingredients
Suboxone contains 80% buprenorphine and 20% naloxone.
- Buprenorphine: an opioid partial agonist, meaning it activates opioid receptors only partially compared to drugs like oxycodone.
- Naloxone: an opioid antagonist or blocker that prevents misuse of Suboxone and discourages relapse.
FAQs: Suboxone Names
Does Suboxone Have a Generic?
Yes, the generic version of Suboxone is called Buprenorphine-Naloxone.
Is Zubsolv The Same As Suboxone?
Zubsolv is another brand for Buprenorphine-Naloxone with higher bioavailability than Suboxone, meaning lower doses are needed. It comes in more dosage options but is typically more expensive.
What Are Other Names for Suboxone?
Illicit street names include Buse, Sobos, Strips, Oranges, Big Whites, Small Whites, Stops, Sub, or Subs. Only use Suboxone from a licensed medical provider. Buprenorphine without naloxone is sometimes referred to as Subutex.
Is Suboxone Substituting One Drug for Another?
No. Suboxone is a medication used to manage opioid addiction, similar to how insulin is used for diabetes. It improves brain function and helps people live normally.
Starting Suboxone
Suboxone should not be taken immediately after opioid use to avoid precipitated withdrawals. It is safe for long-term use.
- Start Suboxone 12-48 hours after last opioid use.
- Initial dosages are standardized; a medical provider should monitor you.
- Dosage is adjusted from day 3 onward.
- To stop, taper the dosage slowly to avoid withdrawal symptoms.
How Do I Take Suboxone?
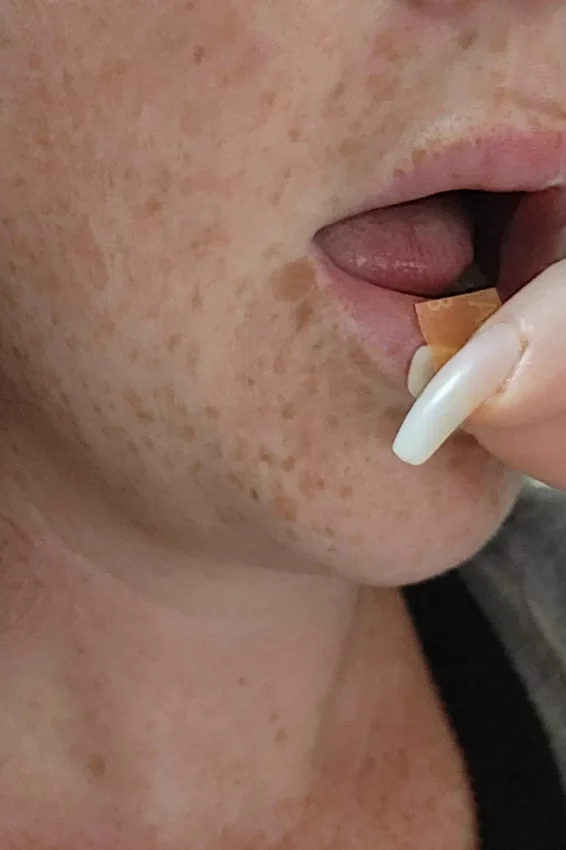
Suboxone is taken as a film placed under the tongue.
Where To Place a Suboxone Film
Place it under your tongue on the bottom.
What Suboxone Looks Like Being Placed Under Tongue
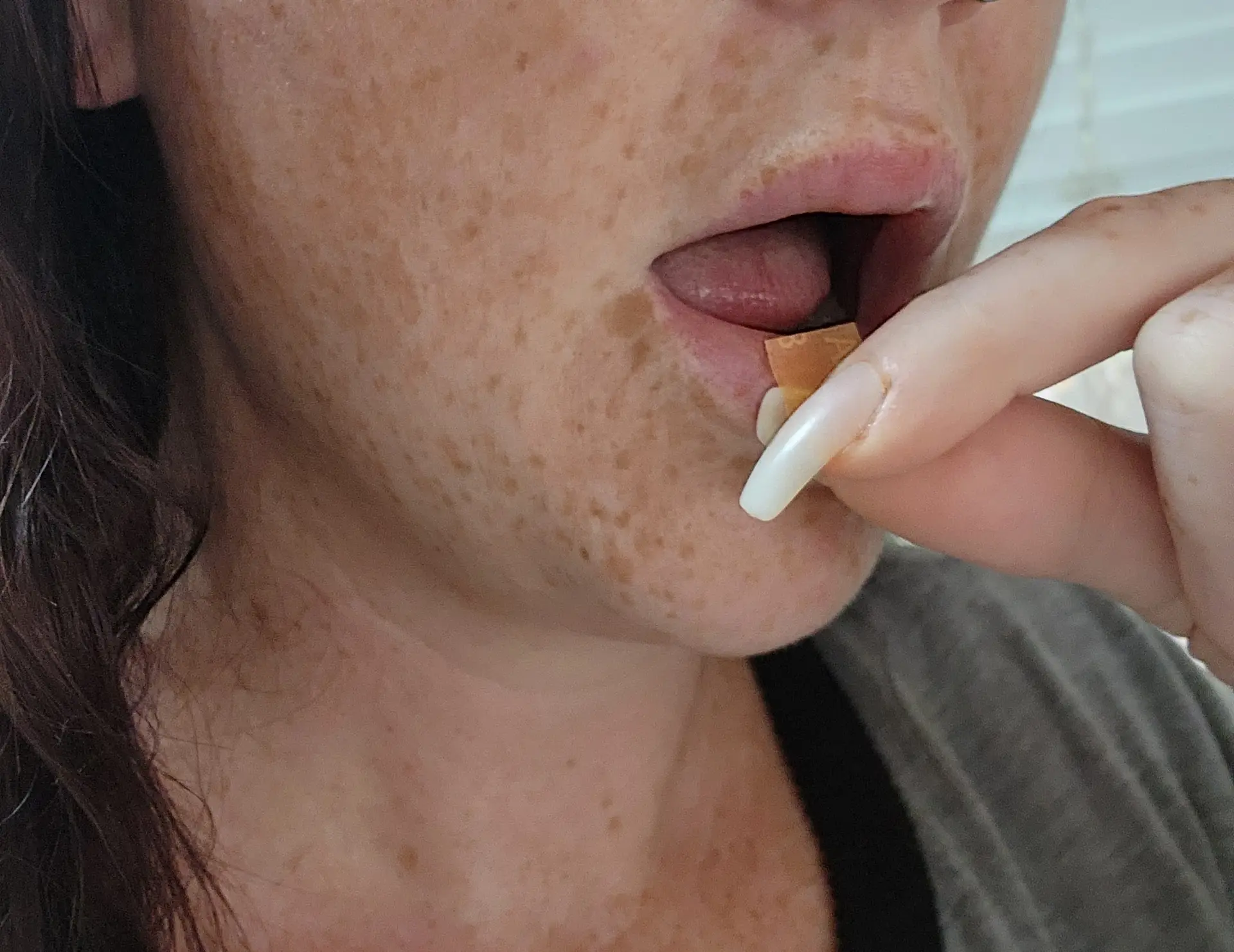
How Long Does Suboxone Take to Dissolve?
About 30 minutes. Avoid eating, drinking, or moving it in your mouth while it dissolves.
Why is Suboxone Sublingual?
It is not well absorbed through digestion. The sublingual route delivers it directly to the bloodstream. Other options include monthly injections like Sublocade.
Why is Suboxone Prescribed?
Suboxone helps treat opioid addiction but is not a cure.
1. Suboxone is only meant for opioid addiction.
- Heroin
- Fentanyl
- Codeine
- Morphine
- Hydrocodone
- Oxycodone
- Methadone
It is not used for alcohol addiction. Vivitrol may be an alternative.
2. Suboxone only treats the physical issues.
Combining Suboxone with therapy helps treat underlying mental health issues like depression, anxiety, or trauma.
Can Suboxone Be Used For Pain?
It’s not FDA-approved for pain but may be used off-label for people with opioid addiction and chronic pain. ⓘ
Methadone is FDA-approved for chronic pain. ⓘ
Side Effects of Suboxone
Suboxone is considered safe. Buprenorphine is recommended even during pregnancy. Most common side effects are constipation and sleep disturbances. Serious side effects are rare. Side Effects of Suboxone
Where to Get Suboxone
Suboxone is usually prescribed at a Suboxone clinic by doctors who specialize in addiction medicine.
- Therapy options: Cognitive Behavioral Therapy (CBT)
- Supportive environment: Non-judgmental, open, compassionate care
Symetria Recovery Suboxone Clinics
Illinois Locations
Texas Locations
Ready for Real Recovery — On Your Terms?
Same-day appointments. Full insurance coverage. No judgment.
Fill out the confidential form and take your first step with Symetria today.
DAP PPC forms - Blog 2026
We respond within 1 business day. Your information is 100% confidential and HIPAA compliant.